
RCP unseen researching the collections
RCP Unseen: researching the collections
Objects from the past can provide unparalleled knowledge that helps us expand our understanding of medicine and society.
As part of living collections, accessible to researchers of any discipline, the objects preserved by the Royal College of Physicians continue to inform and advance scientific, medical and historical research today.
Reproduced courtesy of the Wiley Digital Archives © John Wiley & Sons, Inc. All rights reserved.
Shingles casebook of Henry Head
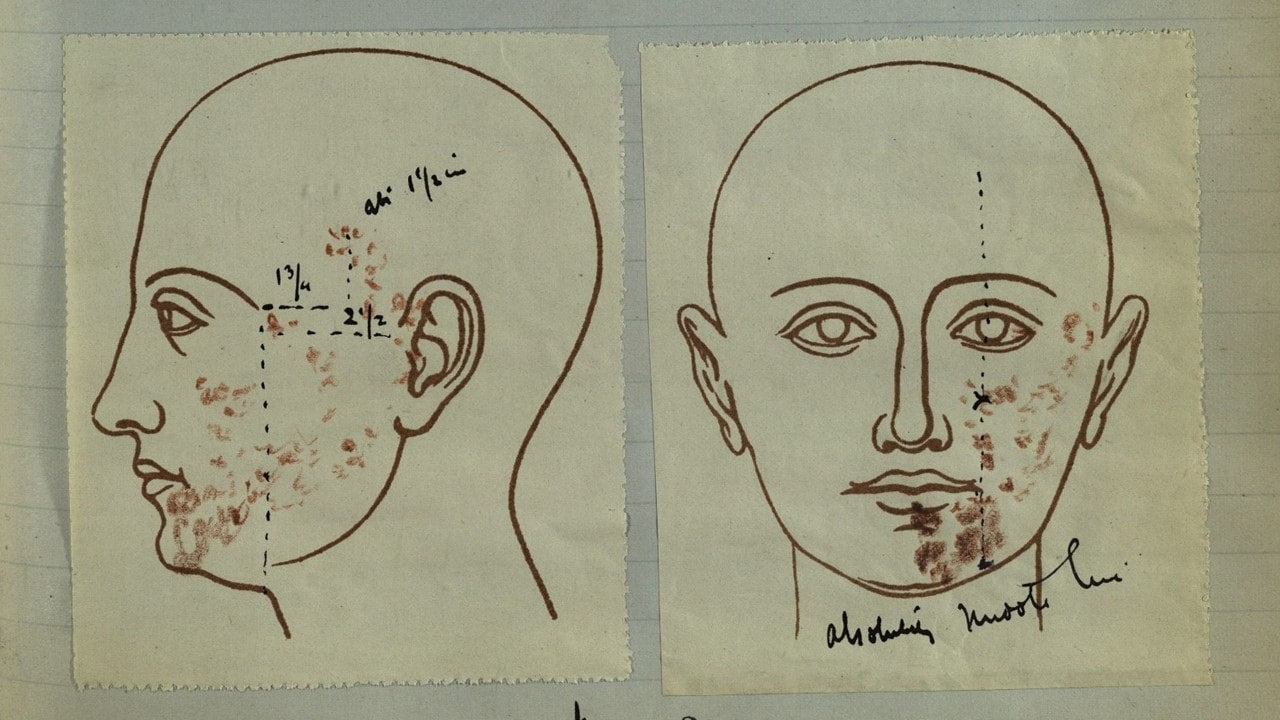
Shingles casebook of Henry Head, London, 1890s (MS330)
When Mrs Staple developed an itchy chin in March 1893, she could not have imagined her case would still be studied almost 130 years later. Hers was one of approximately 500 shingles cases recorded by the neurologist Henry Head (1861–1940), who mapped the layout of nerve cells in the human body by plotting the position of rashes on his patients’ skin.
When researchers Robert Johnson, Andrew Rice, and Sarah Dixon-Smith learned of Head’s notebooks in 2017, they spotted a unique opportunity to study the evolution of shingles. Today, the condition mostly affects older adults, but about 40% of Head’s patients were children. The researchers are painstakingly going through the records, uncovering possible health and social factors influencing this shift in the epidemiology of shingles.

Surgical blade set possibly belonging to Edward Jenner
Surgical blade set possibly belonging to Edward Jenner, London, 1776–1825 (X662)
These blades are helping scientists to learn about the history of smallpox.
‘A Pox In All Our Houses: Discovering the origin and evolution of smallpox vaccine’ is a research project run by McMaster University, Ontario, and the Mütter Research Institute, Philadelphia. Scientists are sampling historic items associated with smallpox vaccination to answer questions about the variety of viruses used for vaccination and to map the spread of smallpox across the globe.
These blades were sampled as they may have been used to vaccinate people against smallpox. A small number of viral molecules have been found in samples taken from the blades, although until further testing is done the virus cannot be fully identified. These blades were probably owned by Edward Jenner (1749–1823), the English doctor who greatly advanced the development of the smallpox inoculation, which eventually led to the global eradication of the disease.
View catalogue entry for Surgical blade set possibly belonging to Edward Jenner
LEFT: Eradicating disease, Video by JD Howell
2 minutes 11 seconds
Postdoctoral fellow Ana Duggan and Professor Hendrik Poinar from McMaster University, Ontario, present their smallpox research project.
McMaster University
Smallpox research

LEFT: Smallpox research, Photograph by Amalia Lemprière
Postdoctoral fellow Ana Duggan from McMaster University, Ontario, undertakes smallpox sampling as part of the research project ‘A Pox In All Our Houses: Discovering the origin and evolution of smallpox vaccine’.
McMaster University
Hear more about the project from Dr Ana Duggan and Anna Dhody director of the Mütter Research Institute, Philadelphia in a recording of our online event Smallpox to COVID: a comparison of vaccine development.
Also featured are curator of the RCP museum Lowri Jones and director of the vaccine research group at the Mayo Clinic, Dr Gregory Poland.
Oral history transcript: Barbara Bannister on smallpox
 Biography:
Biography:
Dr Barbara Bannister grew up in the West Midlands and the New Forest. From grammar school she gained a place to study medicine at the Royal Free Hospital in London. She specialised in infectious diseases and worked as a consultant in the field, setting up an infectious diseases service with J.D Williams at the London and establishing the High-Level Isolation Unit at the Royal Free.
Interviewer: Mike Gibson.
Transcript:
Barbara Bannister remembers one of the last smallpox outbreaks in the UK:
And when I was a houseman, it was in 1973, and there was the outbreak of smallpox in London. And Ronald Emond was the smallpox reference physician and so I saw him out and about at all hours investigating potential smallpox cases. I saw numerous people with side effects of smallpox vaccination, and some of them in hospital, and Ronald took me on a couple of occasions to do domiciliary visits to exclude smallpox, particularly in children. And he was off down to the then Long Reach smallpox hospital to look after the two cases, a woman and her husband, who visited the patient in the next bed to the actual smallpox case. They both died. The man died very quickly of fulminating smallpox, the woman died in what used to be a common course of fatal smallpox. She didn't make it through her second week and she died too. And of course, what did they die of? He died of multi organ failure, just like the viral haemorrhagic fevers that we see from Africa and Asia these days, and she died of what you would say, more progressive organ failure of the sort that you see in intensive care with sepsis cases. But of course with a frightening rash. The man died before he developed a frightening rash.

Glass prism possibly belonging to Sir Isaac Newton
Glass prism possibly belonging to Sir Isaac Newton, 18th century (X654)
Did this prism really belong to Sir Isaac Newton (1642–1727), as our records say?
Prisms of this date are usually made of flint or crown glass, and the two types bend light differently. The differences between the two may explain why some 18th century scientists had trouble replicating Newton’s experiments. Newton’s notes show that he used crown glass, but the RCP prism is made of flint glass, making it unlikely that it belonged to Newton.
This prism is part of a research project led by Yoshimi Takuwa at Tokyo Institute of Technology. ‘Experimental analysis on seventeenth and eighteenth-century optics: mainly on so-called ‘Newton’s prisms’ uses light to determine the type of glass that prisms attributed to Newton and to Newtonian scholar Willem 's Gravesande (1688–1742) are made of. The project aims to increase understanding of scientific experimentation in 17th and 18th century studies of light.
View catalogue entry for Glass prism possibly belonging to Sir Isaac Newton
François Pierre de la Varenne, The French cook
François Pierre de la Varenne, The french cook prescribing the way of making ready of all sorts of meats, fish and flesh, with the proper sauces, either to procure appetite or to advance the power of digestion: with the whole skill of pastry work, London, 1654 (CN20755)
This small book of French recipes was owned by a woman, who wrote her ownership mark on the first and last pages: ‘Elizabeth Ashton her book’. The identity of this owner is still to be confirmed.
Catherine James is studying this book as part of her AHRC-funded PhD research project, ‘Women's ownership of medical knowledge in Tudor and Stuart England, 1485–1714’. James’ research involves surveying all pre-1714 books in the RCP library to look for evidence of women’s involvement in medical practice and care.
Letter from RCP president discussing the creation of the National Health Service
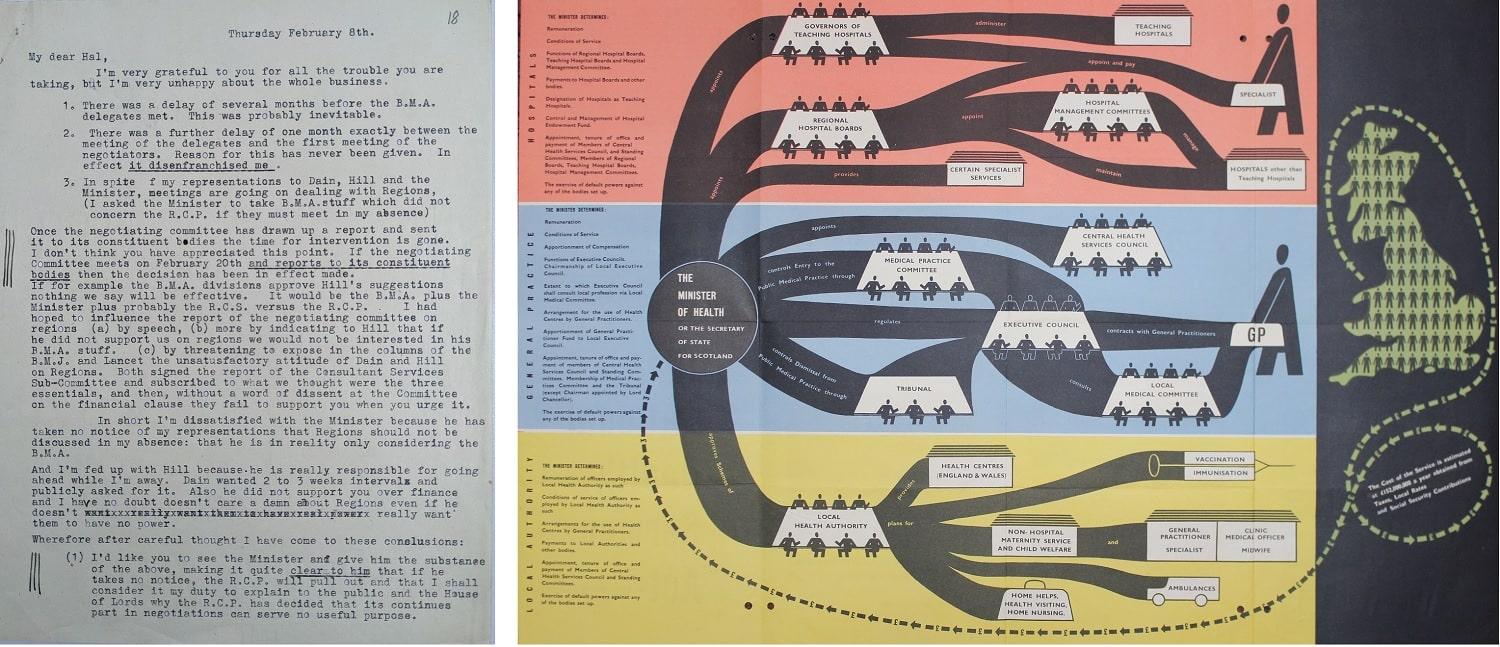
Letter from RCP president discussing the creation of the National Health Service, Yalta, 8 February 1945
MS4434(18)
Charles McMoran Wilson (1882–1977) had a lot on his mind when he wrote this letter. As Winston Churchill’s personal physician, he was responsible for the health of the prime minister at a crucial moment during the Second World War. As a key player in the planning of the new National Health Service (NHS), Wilson was also shaping the future of British healthcare.
Wilson was with Churchill at a conference in Crimea, and his frustration at missing the NHS planning meetings back home is clear in the letter. He worries that in his absence, the interests of physicians will not be represented in the negotiations. However, as the poster next to it shows, Wilson’s fear that the RCP would ‘lose the battle over the regions’ was averted.
In 2018 the NHS celebrated its 70th birthday. Like many other institutions, the RCP took part in conducting research and generating content for the People's History of the NHS blog
Poster showing the proposed structure of the National Health Service (NHS)
Poster showing the proposed structure of the National Health Service (NHS), London, c.1948
MS4363/27
The NHS is now hugely popular with most of the public, but when it was first proposed many physicians and other healthcare professionals were opposed to the idea. One worry was that a system controlled by central government would diminish the role of local expertise.
RCP president Charles McMoran Wilson (1882–1977) played a key role in planning the NHS, as the letter by Wilson in this exhibition also shows. Wilson ensured that physicians from all UK regions were represented in the discussions. The red section of the poster shows that regional hospital boards would have the power to appoint hospital specialists (physicians).
View catalogue entry for the file that includes Poster showing the proposed structure of the National Health Service
Oral history transcript: Lord Moran on the establishment of the NHS
 Biography:
Biography:
Charles Moran was born in Yorkshire and studied medicine at St Mary’s Hospital Medical School, London. He won the Military Cross in 1916 for services during the Battle of the Somme and served as Winston Churchill’s personal physician from 1940 to 1965, an experience that he described in his highly controversial book, ‘The Struggle for Survival’. He was President of the Royal College of Physicians between 1941 and 1949.
Image from the Wellcome collection
Interviewer: Charles Newman.
Transcript:
Charles Moran’s personal memories of the role that the RCP, and he personally, played in the establishment of the NHS:
In the long history of the college it has often influenced the government of the day. Its officers have been high in the confidence of monarchs and their ministers. But times change. A ministry of health was established. A medical research council was appointed. The British Medical Association grew in strength. But the college hardly changed with the times. And war, with its insistent demands made this plain to all. In the early days of the Second World War fellows could not help noticing that the college no longer made any serious or sustained attempt to influence the government of the day on questions arising out of the War, which affected the profession, and the health of the people. There had even been talk in responsible quarters about closing down the college for the duration of the War. And [inaudible 0:01:14] part the college played in the introduction of the National Health Service.
The Royal College of Surgeons represented by Lord Webb-Johnson, said that they were not interested in medical politics, and were not at all helpful. The British Medical Association, actively supported by the general practitioners, was out to destroy the Health Act. The college felt that whatever the faults and deficiencies of the Act it was up to them to improve it and to make it work. The Minister of Health, Aneurin Bevan, irritated by the opposition of the BMA, turned to the college for help in the organisation of a consultant service. The college organised a committee, which was representative of the whole profession, the teaching hospitals, the regional non - teaching hospitals, doctors in government and municipal service, the specialties, and the BMA. It was left to this committee to hammer out the details. It was instrumental in preventing the introduction of a whole time salaried service, and in ensuring that the service was not handed over to the local authorities, to which the profession was fundamentally opposed. In working out the details the college devised the regional scheme. As president I suggested the system of merit awards. In all this the college was carrying out its historic function as the link between the government and the profession.
By 1944 the college was playing a big part in the councils of the nation as far as health was concerned. At that time a luncheon was organised at the Savoy Hotel, at which the Prime Minister, Winston Churchill, proposed a toast to the college, supported by most of the cabinet and the heads of the services. It called to mind the day in 1825 when the new college in Pall Mall East opened its doors to greet five royal dukes and most of the establishment, including the Duke of Wellington. And when the President, Sir Henry Halford, delivered an eloquent oration in Latin. Alas the president of 1944 spoke in his native tongue. I don’t seem to have got any more, that's about it.
Q: [laughs]. What was that lunch, Sir, at the Savoy? Did the college give the lunch?
A: Yes. A terrific meal, we had the prime minister and nearly all the cabinet, all the heads of the services.
Q: Blimey that's splendid. A: Never before, I think has the college spread it so – at that time, as I had Winston Churchill as a patient….
Q: Yes. A: He’d only have to give his word as prime minister and all the rest trooped out –
Q: Yes, yes. A: Because there wasn’t any reason why in busy war time they should have come like they did. But there they were, they were there on block. Q: Well, my gosh, that was even better than Henry Halford’s party! [laughter].
A: Yes.
Oral history transcript: Dr Norman Jones on meeting Nye Bevan
 Biography:
Biography:
Dr Norman Jones grew up in Rumney, Wales. He studied at Christ’s College Brecon and Cambridge University and on graduating secured a position at St Thomas’ Hospital, where he went on to set up one of the country’s first renal dialysis units. He is a former treasurer of the Royal College of Physicians.
Interviewer: Mike Gibson.
Transcript:
Norman Jones shares a childhood memory of being stuck in a train in the Severn Tunnel with Nye Bevan:
Well, I suppose in a funny sort of way my first contact with the NHS in a sense was Nye Bevan. Nye Bevan was the MP for Ebbw Vale, my father was a good friend of the local MP, a non-conformist minister call Llewelyn Williams, and he was a good friend of Nye Bevan. This would have been ‘46, ‘47, ‘48, so very much the foundation of the NHS. And I have one very clear memory of Nye Bevan. In those days the Welsh MPs used to come down for the weekend to their constituencies, and there was a well-known train back to London, to Paddington, on the Sunday late afternoon, evening, I can’t remember what time, but in those days they always used to do any work needed on the Severn Tunnel, through which the train had to go to Paddington, on Sundays and there was always the chance of a hold up. And on one occasion, my father was taking me up to London for some reason, and we were travelling with Llewelyn Williams and Nye Bevan in the same carriage and the train came to a halt in the middle of the Severn Tunnel and the lights went out. And we sat there in the dark for, I don’t know how long, but certainly 15, 20, 25 minutes, and Nye Bevan kept us endlessly amused with a series of stories and so on, and it was memorable. He was a marvellous speaker.
Oral history transcript: John Dornan on his childhood memories of establishment of NHS

Biography:
John Dornan studied medicine at Trinity College Dublin. He qualified in 1965 and joined the Royal Army Medical Corps, serving overseas in both the Middle East and Southeast Asia. On leaving the army he specialised in occupational medicine and worked for the British Steel Corporation and the National Health Service, while continuing to serve in the Territorial Army until 1992.
John Dornan recalls his parents’ anxieties about the impact of the new NHS on their GP practice and how these disappeared once full plans for the service were unveiled.
Interviewer: Val Wood
Transcript:
John Dornan recalls his parents’ anxieties about the impact of the new NHS on their GP practice and how these disappeared once full plans for the service were unveiled:
Well I was eight years old, and father would do his surgery and would then come into the lounge where I would be playing, and he would say to mother, “Have you heard the latest? Aneurin Bevan is going to compulsorily take our practices.” And I know father had borrowed money to buy the practice and was paying it back, and there was no indication then, and don’t forget this is an eight-year-old boy thinking, how the government were going to compensate the doctors for taking over their practices. And I should also say that I thought sometimes when mother and father were sitting in the lounge and I'd be playing with my dinky toys, I could hear them talking, and they were doing the bills that they had to send out to the patients. And they would say, “Poor old Mrs Brown, we've been there three times. But she hasn’t got any money, you can't send her a bill.” So they wouldn’t send her a bill. And then they'd get to Mr Bradley, and they'd say, “Well he's the boss of the local colliery”, this was in Chesterfield, “He's got three Bentleys and whatever, well we’ll just put a bit more on his bill.” And Mr Bradley would be delighted to pay, and Mrs Brown would be delighted that she didn’t have to pay. But it was all finance, and this is an eight-year-old boy taking all this in. The practices were, obviously, taken over, the NHS was born. And I know then my parents continued to work in it for many years and were very pro, as most doctors were. And the one day I do remember is my father rushed into the lounge with a letter, and he said, “Good heavens,” this was to my mother, “They are going to pay us,” and I can't remember what it was. I was probably a year older then, nine or something. He said, “I never would have believed the government would have paid us that amount of money for the practice.” And straight away his worries, concerns, and anxieties were over.
Part of the exhibition 'RCP Unseen'. Explore further:


