
Muriel Buxton-Thomas (1945 – 2016), was an internationally recognised physician in the field of nuclear medicine - the branch of medicine that deals with the use of radioactive substances in research, diagnosis, and treatment. She was an active contributor to academic and clinical research throughout her career.
Born in Freetown, Sierra Leone, Buxton-Thomas moved with her family to London in 1955. She studied at Newcastle Medical School, qualifying in 1971. She accepted a medical registrar rotation at St Thomas’ Hospital, London, following house jobs in Newcastle, where she spent time in the nuclear medicine unit. The specialty of nuclear medicine became her life’s work and she was awarded the London MSc in nuclear medicine in 1978.
First a senior registrar in nuclear medicine at Addenbrooke’s hospital Buxton-Thomas went on to be a consultant physician in the specialty at St Thomas’ and Medway. From 1992 she worked at King’s College Hospital becoming clinical director of nuclear medicine. Her clinical work included many specialties such as adult and paediatric hepatology, osteoporosis, pulmonary medicine and endocrinology.
While making a success of her busy clinical appointments Buxton-Thomas enthusiastically continued with clinical research, publishing more than 50 research papers and three books. An active contributor to many nuclear medicine meetings throughout the world, her research work also generated over £250,000 in research grants.
Buxton-Thomas served on many committees, holding important national roles for the Department of Health and the Administration of Radioactive Substances Advisory Committee (ARSAC). She was also instrumental in setting up the King’s College, London, MSc in nuclear medicine.
She made it clear that she did not accept the second rate and was a vocal advocate for her department and the patients it served. The description ‘formidable’ has been applied to her character, but this appearance hid a sympathetic, kind and generous person who could not tolerate deception and who had an abiding Christian faith.
Edward Howard, Inspiring Physicians, Royal College of Physicians
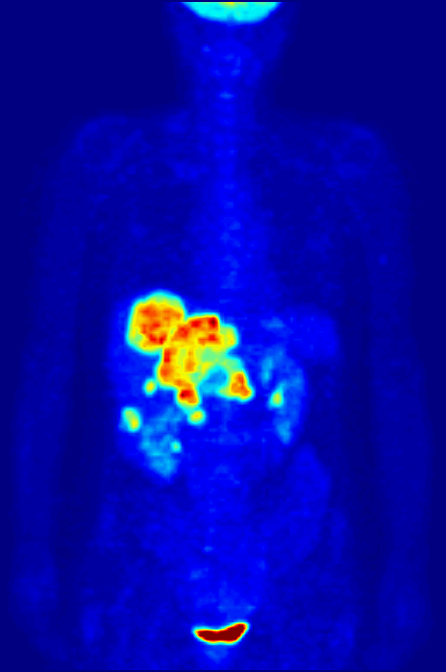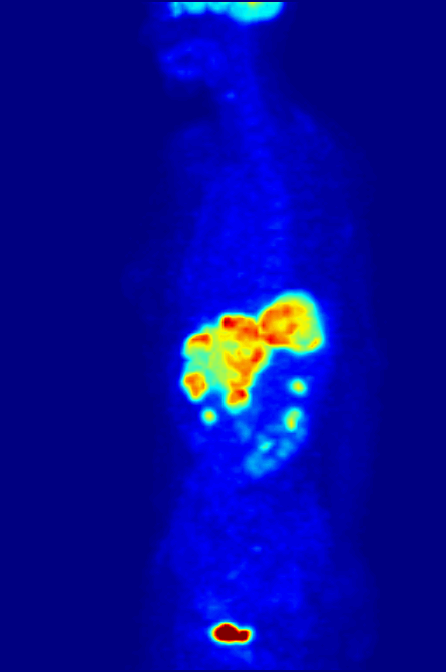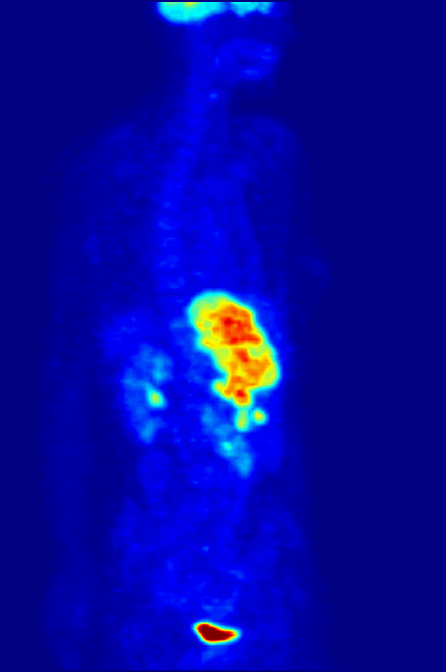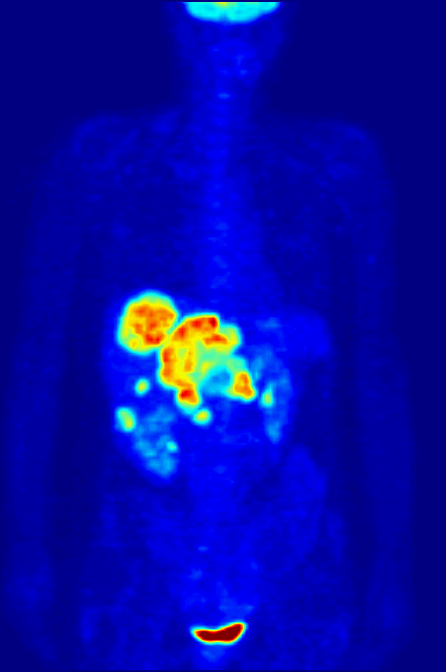
‘Exceptional contribution to nuclear medicine’
While working as an extremely busy clinician in the field of nuclear medicine, Buxton-Thomas became an internationally recognised leading expert contributing significantly to the development and introduction of new diagnostic methods and therapies.
At King’s College hospital she was instrumental in the installation of one of the first PET gamma cameras in England and the relocation of the Nuclear Medicine department to the new Golden Jubilee Wing.
Positron emission tomography, or PET scans, are used to provide detailed 3-dimensional images of the inside of the body. They work by detecting the radiation given off by a radiotracer injected into the patient. By analysing the areas where the radiotracer does and doesn't build up, it's possible to work out how well certain body functions are working and identify any abnormalities like cancerous cells.
She also worked on many areas of clinical research including the development of peptide receptor radionuclide therapy (PRRT) using radio-labelled somastatin analogues. This is a targeted cancer therapy used in the treatment of neuroendocrine tumours (NETs). NETs are rare tumours that can develop in many different organs of the body. They affect the cells that release hormones into the bloodstream (neuroendocrine cells). PRRT has been called a ‘magic bullet’ treatment.
"In PRRT, a cell-targeting protein (or peptide), similar to the natural circulating hormone somatostatin, is combined with a small amount of radioactive material, or radionuclide, creating a special type of radiopharmaceutical called a radiopeptide. When injected into the patient’s bloodstream, this radiopeptide travels to and binds to neuroendocrine tumor cells, delivering a targeted high dose of radiation directly to the cancer cells. The mechanism by which this radiopeptide can target the tumor cell is the abundance (called an overexpression) of a specific type of surface receptor—a protein that extends from the cell’s surface—that binds to somatostatin."
Society of Nuclear Medicine and Molecular Imaging
You can still watch a lecture Buxton-Thomas gave discussing the developments made, and ongoing progress, with certain types of cell-targeting peptides and radionuclides for treatments back in 2008.
Watch Buxton-Thomas' lecture on YouTube
After her retirement in 2010 she worked closely with colleagues at the Birmingham Neuroendocrine Tumour Centre to secure its status as a centre of excellence certified by the European Neuroendocrine Tumor Society providing therapies such as PRRT.
In 2017 Buxton-Thomas was posthumously awarded the Presidents’ Medal from the British Nuclear Medicine Society which is given for the ‘exceptional contribution to nuclear medicine’. The medal was received by her daughter, Dr Rachel Buxton-Thomas, consultant respiratory physician at Brighton and Sussex University Hospitals.
Gail Chapman, public programmes officer
Sources used in writing this post:
- Howard, E. Muriel Simisola Buxton-Thomas, 2017. https://history.rcplondon.ac.uk/inspiring-physicians/muriel-simisola-buxton-thomas [Accessed 27 August 2020].
- British Nuclear Medicine Society. Obituaries Dr Muriel Buxton-Thomas 1945-2016
- www.bnms.org.uk/obituaries/dr-muriel-buxton-thomas-1945-2016.html [Accessed 27 August 2020].
- University Hospitals Birmingham. Birmingham NeuroEndocrine Tumour Centre, 2020. https://www.uhb.nhs.uk/birmingham-neuroendocrine-tumour-centre.htm [Accessed 27 August 2020].
- Society of Nuclear Medicine & Nuclear Imaging. Fact sheet: What is Peptide Receptor Radionuclide Therapy (PRRT), 2018. https://www.snmmi.org/AboutSNMMI/Content.aspx?ItemNumber=29883 [Accessed 27 August 2020].
- University Hospitals Birmingham Charity. ‘Magic bullet’ treatment comes to Birmingham, 2013. https://www.hospitalcharity.org/news/magic-bullet-treatment-comes-to-birmingham [Accessed 27 August 2020].
- Wikipedia. Positron emission tomography, 2006. https://en.wikipedia.org/wiki/Positron_emission_tomography#/media/File:PET-MIPS-anim.gif [Accessed 27 August 2020].
- NHS. Neuroendocrine Tumours, 2017. https://www.nhs.uk/conditions/neuroendocrine-tumours/#:~:text=A%20neuroendocrine%20tumour%20is%20a,grow%20slowly%2C%20but%20not%20always. [Accessed 28 August 2020].
